What is the TMJ?
TMJ is the abbreviation for temporomandibular joint. Everyone has two of these joints, and the term “TMJ” refers to the normal, healthy joint on each side of the skull that allows the lower jaw to function during speech, swallowing, and chewing. The name of the joint comes from the two bones that make up each side of the joint. Like all joints, the TMJ is made of muscle, ligaments, cartilage, and bone with supporting nerves and nutritional supply in the form of synovial fluid.
The temporal bones of the skull form the “roof” and “inside” of the TMJ, and the mandible (lower jaw) makes up the floor of the joint, which moves in three directions: It rotates around an imaginary axis for the first part of the opening stroke of the jaw and the last part of the closing stroke; it translates , or slides, down and forward from the endpoint of rotation to maximum jaw opening; and, it moves side to side. Specifically, the part of the mandible that is involved with the TMJ is called the condyle, and the part of the temporal bone involved in the joint is called the temporal fossa. Because the TMJ moves in three planes of space, unlike all other joints in the body that move like a hinge, the TMJ is called a ginglymoarthroidal joint. Between the two bones is a cartilaginous disc that serves as sort of a shock absorber to protect the joint that slides with the condyle during the range of motion. Attaching to the disc and the mandible is a specific muscle, called the lateral pterygoid that pulls the disc and the jaw forward as the jaw translates. There also ligaments that hold the disc to the condyle on each side of the disc, called collateral ligaments.
A discussion of the TMJ is not complete without mentioning that the mandible is essentially a bone floating in space. In fact, when ancient skulls are discovered in archaeology, the mandibles are usually absent because the soft tissue has all been lost, allowing separation of the mandible from the skull.
This means that the function, health, and stability of the TMJ is totally dependent on the supporting muscles and ligaments of the head and neck and the teeth that provide a stop at the right place for optimal chewing strength.
The masseter muscles, the temporalis muscles, the digastric muscles, the medial pterygoid muscles, and the lateral pterygoid muscles are the primary muscles involved in jaw function. Since these muscles all work by pulling on the bones of the skull, it is important to consider that the skull is like a bowling ball balancing on a broken broomstick, which is the spine. This balancing act requires harmony in function of many supporting muscles of the upper back, neck, chest, and shoulders. Therefore, it is easy to understand how many problems of the head, neck, and upper back can manifest themselves as TMJ problems; sometimes, TMJ problems can also present as dental problems, neck pain, headaches, etc. Often, the term “TMJ” is incorrectly used to refer to a problem that does not easily fit another diagnosis by the medical community.
What is TMD?
When any part of the anatomical structures or supporting structures of the TMJ is injured or damaged, dysfunction occurs. While “TMJ” refers to the temporomandibular joint itself, “TMD” refers to temporomandibular disorder. TMD syndrome is a vague term that usually involves one or more conditions listed below and/or others not mentioned:

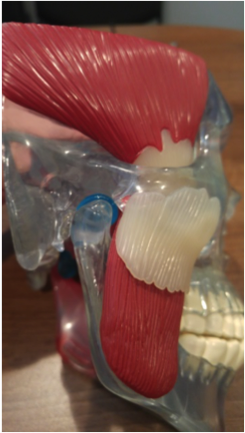
This model represents and injured TMJ where the disc (blue) is displaced and the condyle is degenerating. Capsulitis
- Tendonitis
- Myofascial pain
- Myositis
- Myalgia
- Osteoarthritis
- Degenerative Joint Disease
- Retrodiscitis
- Tinnitis
- Headaches of various types
- Dislocation of the disc
- Subluxation of the disc
- Muscle spasm
- Cervicalgia
TMD Treatment
Treatment for TMD is dependent on the specific diagnoses involved and is typically directed to resolving pain rather than reducing joint noises (popping, clicking, etc.). Joint noises are evidence that injury has occurred and are signs rather than symptoms. Pain, compromised quality of life, and compromised function, however, are symptoms that treatment is typically directed toward.
Treatment for TMJ disorders is controversial, and clinicians often differ in their approach. Some tend to treat physically (physical therapy, bite splint therapy, chiropractic, etc.), some tend to approach treatment from a medical model (medications, mental health therapy, etc.), and some practice the philosophy that TMD tends to be self-limiting and opt not to treat but rather provide supportive care only.
The reality is that successful management of TMD usually involves elements of each approach and often requires a team approach involving some or all of the following healthcare providers: dentist, mental health specialist, family physician, physical therapist, chiropractor, massotherapist, orofacial pain specialist, oral surgeon, etc.
Because TMD is often a chronic pain disorder, compromises in mental health in the form of depression, anxiety, psychosomatic conditions, all of which may require the assistance of a psychiatrist.
Dentists often use bite splints to treat TMD syndrome
The type of splint used should be dependent on a specific diagnosis of a specific condition. For this reason, different types of splints may be used at different times during the treatment of TMD. In fact, splints may actually also be used for diagnostic purposes to rule out complicating factors.
Additional Information on TMJ & TMD
Do I Have TMJ?
When someone has jaw pain, pain in or around the ear, and/or popping or clicking in front of the ear, they’re likely to ask their dentist if they have “TMJ.”
However, this isn’t technically the right question to ask, since EVERYONE has TMJ—two of them, to be accurate.
The term TMJ is an abbreviation that refers to the jaw joint, known as the temporomandibular joint. Everyone has these joints, and they allow us to chew, swallow, speak and keep our airways open.
When someone asks if they have “TMJ,” it is more likely that they have a temporomandibular disorder, or TMD. Even then, TMD is a broad term and not a diagnosis of a specific disorder. There are many possible issues that fall under this blanket, each which may require a different type of treatment (if they require treatment at all)—muscle injuries, bone problems, inflammation of blood vessels, etc.
Most patients with a temporomandibular disorder will have more than one of these, and, for best results, they will require treatment that targets each of the issues that contribute to their symptoms.
Treatment for TMD
Initial treatments for temporomandibular disorders typically include self-care regimens assigned by your provider, exercises, behavioral therapy, physical therapy, bite splints (“nightguards”), and the like. Various medications may also be prescribed, including antidepressants, anti-inflammatories or muscle relaxants. Dietary supplements can help as well. Caution: Athletic-type mouthguards and store-bought bite splints may cause significant injury in many types of TMD and should never be recommended.
It’s only after these options have been explored that more permanent options such as bite adjustments or surgical proceeders will be considered.
A thorough diagnosis of TMD involves an in-depth review of the patient’s medical and dental history, including looking for risk factors for sleep disorders and psychological risks, as well as a thorough physical exam of the head and screening of cranial nerves. Imaging like panoramic x-rays, conebeam CT, and MRI are usually considered and used as appropriately indicated. As there are over forty recognized diagnoses that fall under “TMD,” a thorough approach is required in order to find the source(s) of the problem before an appropriate treatment plan can be developed.
Being told you may have TMD is a starting point, but isn’t enough to determine the best course of treatment for you. If you’ve suffered from any of the symptoms we described above and have ineffective treatment in the past, it’s very likely that you may need a more accurate diagnosis of the real problems behind your pain. Make an appointment with Dr. Huff to find out what a specialist in orofacial pain can do for you.


